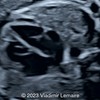
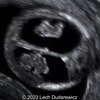
Case of the Week (COW)

Current Case of the Week (COW)

Current Case of the Week (COW)
The kids were tired of hiking in volcanos so we promised them a lazy day at the beach
Submit Your Answer
To join the community and participate in solving current cases, simply click the "view current case" button below. This will take you to the case summary page with full details and additional media. To participate, you will first need to create an account or sign-in. You can then submit your answers.
You can only submit your answers once, but you get three answers. The correct answer is revealed at the end of the posting period.
Physicians
Previous Winners
No one has answered correctly yet! Check back soon.
First-Time Winners
No one has answered correctly yet! Check back soon.
Sonographers
Previous Winners
No one has answered correctly yet! Check back soon.
First-Time Winners
No one has answered correctly yet! Check back soon.
Contributors
Top Contributors
No contributors yet! Check back soon.
Previous winners: Users who have been recognized on a "Top Winners list" in years past; First-time winners: Users who have not yet been on the annual "Top Winners list." The Sonographers category also incorporates "other" job titles.

News & Notes
Dear Esteemed Users of TheFetus.net,
Thank you to everyone who participated in the Case of the Week in 2023. There were many challenging cases and 266 people answered at least one case correctly. Congratulations! Please continue to tell your colleagues about TheFetus.net so that we can reach more people with free education about fetal medicine.
We have finalized the annual winner's list that recognizes those who have persistently found the correct diagnosis to the Case… read the full entry
TheFetus.net